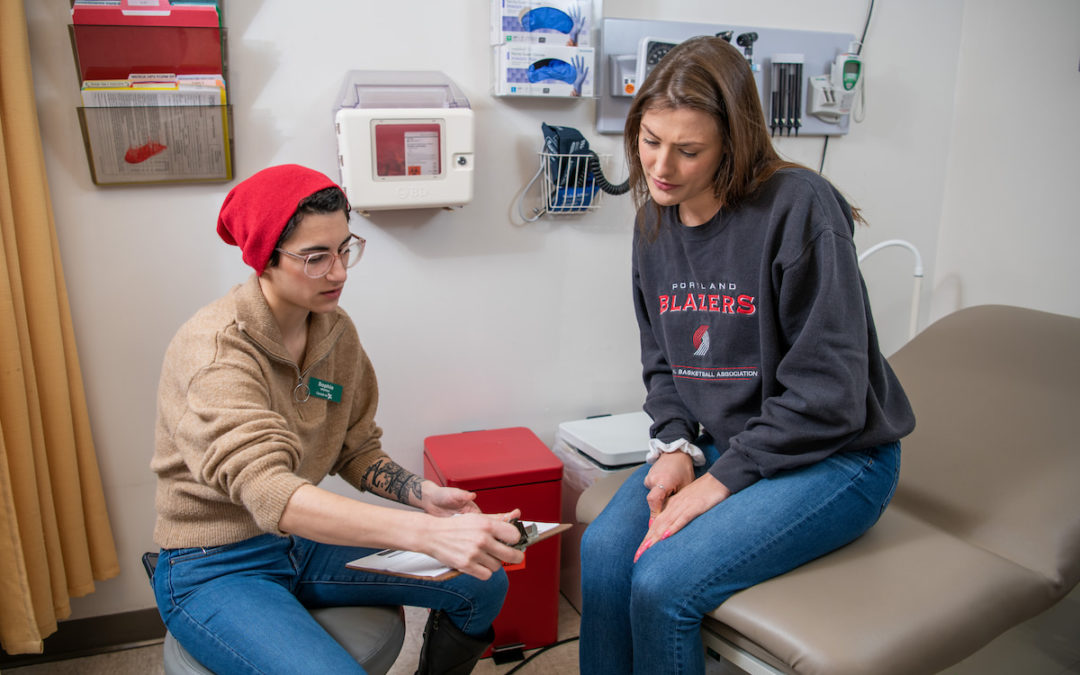
“As a clinician, I start with the assumption that everyone has experienced trauma. And when I walk into an exam room to meet a patient for the first time, I have no idea what that trauma might be.”
Trauma-Informed Care is Integral at Outside In
Here are Outside In, we often talk about incorporating trauma-informed care throughout our services. But what is trauma-informed care, and what does it look like at Outside In. To help us learn more, we spoke with Kathleen Walker, a Nurse Practitioner at Outside In, and Alli Diament, who is our Medication Assisted Treatment Program Coordinator.
But first – what is trauma-informed care? It starts with a baseline assumption that we have all experienced some level of trauma. It is being aware that many people have had traumatic experiences, having an understanding of how trauma affects people, and creating environments where people have the ability to feel safe.
What Does Trauma-Informed Care Look Like at Outside In’s Clinic?
Kathleen shared more about how she incorporates trauma-informed care into patient visits.
“As a clinician, I start with the assumption that everyone has experienced trauma. And when I walk into the exam room to meet a patient for the first time, I have no idea what that trauma might be.
There has been a lot of research done on allowing space for patients to share their trauma, without re-traumatizing them. So, I start by creating a safe space, without digging into details.
Many patients have had negative experiences with the health care system or a past health care provider. I let patients know that if at any point they’d like to share more about that, I’m here for that. I find that opening the door with an open-ended question can be helpful, and lets the patient know that they are welcome to share if and when they feel inclined.
I also always ask patients for permission before I do part of their exam, and I don’t ever make assumptions about what will trigger a patient’s past traumas. Asking patients, “Do you mind if I do this?” helps to build trust. So, if someone comes in with a cough, I might first tell them why I think a chest and lung exam is appropriate and then ask permission to do that exam. Asking a patient for permission rather than telling a patient what you’re going to do makes a big difference if the patient has had past traumas.
If it is a sensitive exam, such a pelvic exam, I ask them how they feel about it, if they are comfortable with the exam, and if there is anything they want to share with me. Before an exam, I explain the steps that will be involved in the exam, and I always try to tell patients that their safety is the most important thing. If they feel triggered or unsafe and need an exam to stop, that takes precedence over finishing the exam. Because if we lose trust, then the patient won’t come back.
Finally, trauma-informed care involves shared decision making with the patient. We create a plan together, and they are integrally involved in their care and treatment plan.”
Trauma-Informed Care is Critical to OI’s Medication Assisted Treatment Program
Alli shared that she always uses a lens of trauma-informed care in her work with patients with substance use disorders who are participating in Outside In’s Medication Assisted Treatment (MAT) Program. Many of her patients have experienced trauma – often many traumas. For her, it’s important to remember and be aware of how things like a patient’s race, class, sexual orientation, gender identity, weight, and disability can impact their life experiences. Often, patients in the MAT program have had past negative experiences with the health care system, and Alli listens to and validates their experiences, and really hears the patient.
Patients in the MAT program have been through a lot, and Alli celebrates every victory – no matter how big or small. We acknowledge anything that a client does that is a step in a positive direction. Patients often use substances to cope, and Alli works with them to find different and more positive coping skills. We don’t expect people to be perfect, and we always accept patients and do not judge them. We are consistent with our expectations, but also flexible and understanding of the stressors that our patients live with every day. And when lapses happen, we don’t judge them for that. We talk about it, and we talk about what could be done differently in the future. We make sure our patients know that they are not failures. They have a struggle, and that’s okay, and we help them to move forward in the direction of their choosing.
Benefits of Trauma-Informed Care
We asked Alli about the benefits of providing trauma-informed care to our patients and clients. She said that her patients often tell her that they finally feel respected and heard when they come to Outside In, and they express gratitude for us being able to help them, rather than judging them or giving them sub-par care. Alli works with patients with substance use disorders, and many of her patients have had negative experiences with other health care providers. They often report feeling judged and treated differently when they have accessed care in other places. But at Outside In, patients feel like our staff respects and understands their lived experiences and the ways trauma can impact someone’s behavior and life experience.
Resources on Trauma-Informed Care
Everyone can apply trauma-informed care in their spaces. And any place, including workplaces, can do things in a more trauma-informed way. Alli and Kathleen have shared some resources for people who want to learn more!
The Curbsiders Podcast: Trauma-Informed Care with Megan Gerber, MD
Trauma-Informed Care – Making it Stick (Relias)
What is Trauma Informed Care (OHA)
Road Map to Trauma Informed Care (Trauma Informed Oregon)
Trauma Informed Care Project Related Website (The Trauma Informed Care Project)
Thank you!
It is because of you – our community –
that Outside In is able to save the lives of thousands of people each year.
We would love to hear from you!
Please feel free to share your thoughts, ideas, and questions with us.
We are grateful for your support!